6 oxygen tanks
1 O2 saturation monitor
1 nebulizer machine do-dad
1 feeding pump
1 iv pole
A wagon full of accessories and attachments.
This is the goody bag we are leaving the hospital with! I know, right?! It's ok, you can be jealous. All you probably get when you leave is a receipt for your ER copay. If you stay in the hospital for 9 days, you get fun stuff like this.
We go home today. We haven't left yet, but the docs came by and confirmed we get to leave. So, what has happened since...
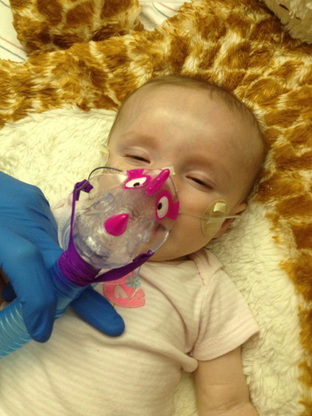
The doctor team really took on a new approach from saturday to sunday. They realized this is a bigger situation than we all origianlly thought. Due to Bentley's muscle weakness and lack of a strong desire to eat everything we need to give her, her ability to recover from this lung thing was impacted. We have started, and will continue, rigorous respiratory therapy stuff. Mainly in the form of nebulizer treatments, and chest PT. The congestion and inflamation from her bronchiolitis inhibits gas exchange in her lungs. This is why we are going home on oxygen and continuing those therapies for now. The oxygen should be a relatively temporary thing. But as all our docs have reaffirmed, this could take weeks or months to recover from, even for a baby without some of her possible probs.
Nutrition-wise, we need to monitor B's caloric intake. We have gone from the 50th percentile down to less than 3rd percentile. Remember those bell curves you studied back in school, yeah, she's down on the lower left corner where it's really small. We need to get her back up. So B has a Nasogastric tube in place. This is a small tube the size of a spaghetti noodle going through her nose into her stomach. We will supplement anything she doesn't consume by mouth through the tube. Ex: We have a target of 5oz per bottle, if she takes 3oz from her bottle and stops, we give the remaining 2oz through tube. Plus overnight continuous feedings to help build her back up. Idealy this will be a temporary thing too. To help her get back to where she needs to be. Although, our team of docs seem to think it may be more long term. We have already discussed the plan for a gastric tube, if it becomes a necessity.
I have to give a big shout out to our doctors, nurses, and respiratory therapists here at Children's. They have been great. We've had awesome care. Multiple nurses deserve the Daisy Award. I love having a team of residents coming in. One of them stops by many times per day. And you have a chance to teach them something.Our attending doc has been fantastic and the residents and interns have probably learned as much about deaf and blind babies as we have about babies on oxygen and tube feeds. Lindsay has done a good job of letting them know things work deferently with B, focusing on her need for consistency and routine. The RT's here have really impressed me as well.
Well, our lives keep changing. A week and a half ago I had a very different outlook for the months of April, May, and June. Today I know flexibility is an understatement. Adjustment is daily. Sanity is relative. Our reality is ours. We must rely on each other and our friends and family more than ever. Thank you, in advance, for what we may ask for.
Snakes and airplanes, that's what scares me. Having the privilege to be my child's nurse, shoot, that's just fun!


 RSS Feed
RSS Feed
